Understanding Eczema Treatment: A Comprehensive Guide to Healing Your Skin
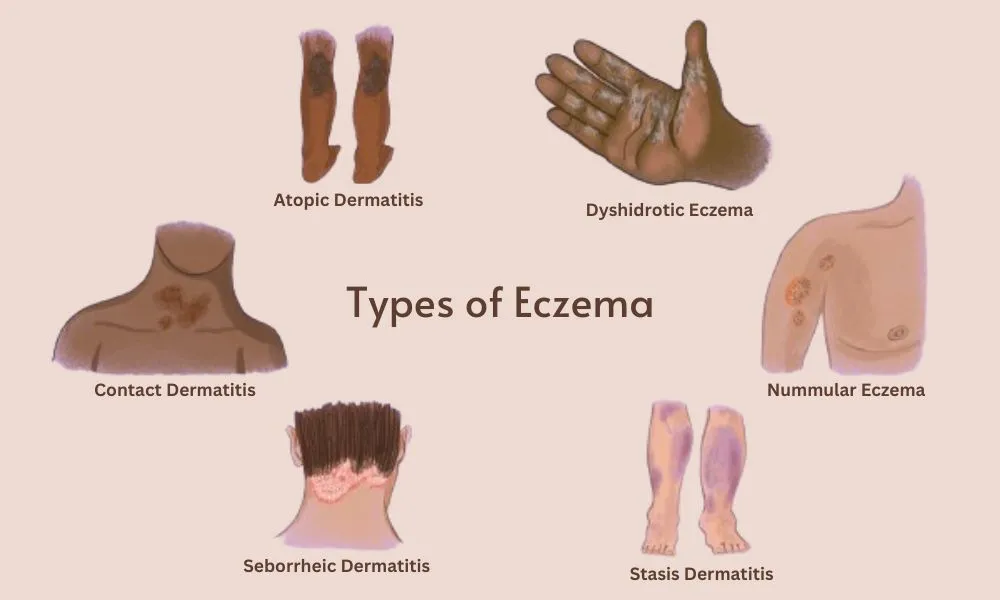
Eczema, medically known as atopic dermatitis, is more than just "dry skin." It is a complex, chronic inflammatory condition that affects millions worldwide, characterized by intense itching, redness, and a compromised skin barrier. Finding an effective eczema treatment requires a multi-faceted approach that evolves over time as science advances and as an individual’s skin needs change. This guide explores the journey from immediate relief to long-term management.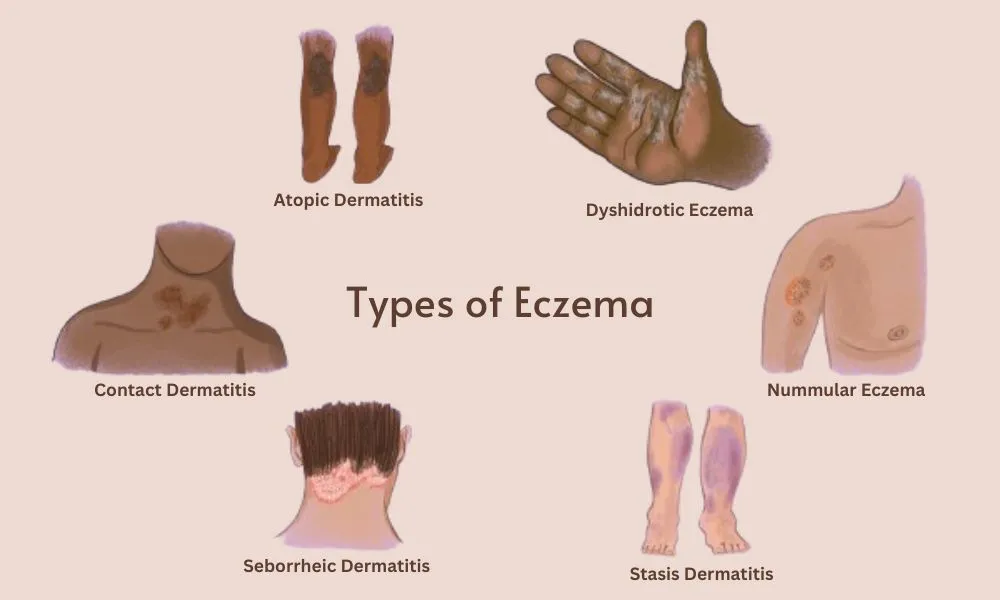
1. The Immediate Response: Relieving Acute Symptoms
When an eczema flare-up begins, the primary goal of eczema treatment is to break the itch-scratch cycle. The skin becomes inflamed, leading to microscopic tears that allow irritants and bacteria to enter. Immediate intervention usually involves topical corticosteroids to reduce inflammation quickly and prevent the rash from spreading or becoming infected.
Beyond medication, the first 24 hours of a flare-up require a "back to basics" skincare routine. This involves eliminating all fragranced products and switching to hypoallergenic cleansers. Applying a thick layer of emollient or petroleum jelly immediately after a lukewarm shower helps seal in moisture, providing a physical barrier that the skin currently lacks.
Essential First Steps for Flares
- Identify Triggers: Look for recent changes in soap, detergent, or diet.
- Cool Compresses: Use a clean, damp cloth to soothe burning sensations.
- Antihistamines: While they don't stop the eczema itself, they can help with the sedative effect to ensure better sleep during a flare.
2. Establishing a Daily Maintenance Routine
Consistency is the cornerstone of long-term eczema treatment. Unlike healthy skin, eczema-prone skin loses moisture rapidly through transepidermal water loss (TEWL). A daily maintenance routine isn't just about pampering; it is a medical necessity to repair the stratum corneum, the outermost layer of the skin.
This routine typically centers on the "soak and seal" method. Patients are advised to bathe in lukewarm water for 10 minutes and then apply ceramide-rich moisturizers within three minutes of patting the skin dry. Ceramides are lipids naturally found in the skin that people with eczema often lack, making their replenishment vital for barrier repair.
3. The Role of Topical Prescription Therapies
When over-the-counter lotions aren't enough, doctors prescribe targeted eczema treatment options. Topical calcineurin inhibitors (TCIs), such as tacrolimus or pimecrolimus, are non-steroidal alternatives that work by suppressing the overactive immune response in the skin. These are particularly useful for sensitive areas like the face and eyelids where steroids might cause skin thinning.
Another modern breakthrough in topicals is PDE4 inhibitors. These non-steroidal creams work inside the skin cells to block the enzyme phosphodiesterase 4, which contributes to inflammation. By diversifying the types of topical treatments used, patients can manage chronic symptoms without the long-term side effects associated with continuous steroid use.
Common Topical Categories
- Low-potency steroids: For mild areas or children.
- High-potency steroids: For thick, lichenified (leathery) skin.
- JAK inhibitors (topical): A newer class that targets specific signaling pathways.
4. Understanding Trigger Identification and Avoidance
Long-term eczema treatment is as much about what you don't put on your skin as what you do. Environmental triggers can range from dust mites and pet dander to seasonal pollen. Many patients find that keeping a "skin diary" helps them correlate flare-ups with specific environmental factors or high-stress periods.
Contact irritants are also a major hurdle. Common culprits include sodium lauryl sulfate (found in many soaps) and synthetic fragrances. Switching to 100% cotton clothing and using double-rinse cycles for laundry can significantly reduce the chemical burden on the skin, allowing the natural healing process to take place more effectively.
5. Phototherapy: Harnessing the Power of Light
For patients with moderate-to-severe eczema who do not respond well to creams, phototherapy (light therapy) is a highly effective eczema treatment. This involves exposing the skin to controlled amounts of Narrowband Ultraviolet B (NB-UVB) light. The light waves help reduce the inflammatory response and can even boost the skin's natural antimicrobial peptide production.
Phototherapy usually requires visiting a clinic two to three times a week. Over a period of several months, the skin's appearance improves, and the frequency of flares decreases. It is often used as a "bridge" therapy to get a patient's skin under control before transitioning back to a strictly topical regimen.
6. Advanced Systemic Treatments and Biologics
In the last decade, eczema treatment has been revolutionized by biologic medications. Unlike broad immunosuppressants, biologics like Dupilumab target specific proteins (interleukins IL-4 and IL-13) that are responsible for the underlying inflammation in atopic dermatitis. This "precision medicine" approach allows for clearing the skin with fewer systemic side effects.
For those who prefer oral medications, JAK inhibitors (Janus kinase inhibitors) have emerged as a powerful tool. These pills work by interfering with the signals that tell the immune system to create inflammation and itch. While these systemic therapies require closer monitoring by a dermatologist, they offer life-changing relief for those with refractory eczema.
7. Natural and Integrative Approaches
Many individuals seek a holistic eczema treatment to complement their medical prescriptions. Coconut oil, for instance, has been shown in studies to reduce the presence of Staph bacteria on the skin while providing hydration. Similarly, colloidal oatmeal baths are a time-honored way to soothe irritation and restore the skin's pH balance.
Dietary changes are frequently discussed in the eczema community. While not everyone has a food-triggered flare, some find relief by following an anti-inflammatory diet rich in Omega-3 fatty acids (found in salmon and flaxseeds) and probiotics. These "gut-skin axis" interventions aim to lower the overall systemic inflammation in the body.
8. Managing the Psychological Impact of Eczema
Effective eczema treatment must address the mind as well as the body. The "itch-scratch-anxiety" cycle is real; chronic itching can lead to sleep deprivation, which increases stress, which in turn triggers more eczema. Cognitive Behavioral Therapy (CBT) and habit-reversal training are increasingly used to help patients stop the subconscious urge to scratch.
Support groups and counseling provide an emotional outlet for the frustration that comes with a visible skin condition. Addressing the mental health component of eczema can improve a patient’s adherence to their skincare routine and overall quality of life, making it an essential pillar of a comprehensive treatment plan.
9. Pediatric Eczema: Special Considerations for Children
Treating children requires a gentler touch and a focus on long-term safety. Pediatric eczema treatment emphasizes "wet wrap therapy," where a medicated cream is applied, followed by a layer of damp gauze and a dry outer layer. This increases the absorption of the medication and prevents the child from scratching the area during the night.
Education for parents is vital. Understanding that eczema is not contagious and that it often improves as the child's immune system matures provides much-needed hope. Doctors often focus on maintaining the acid mantle of a child's skin through soap-free cleansing to prevent the development of other allergies, a phenomenon known as the atopic march.
10. The Future of Eczema Care and Prevention
The landscape of eczema treatment is rapidly shifting toward prevention and personalized care. Researchers are currently investigating microbiome transplants, where "good" bacteria are applied to the skin to crowd out harmful pathogens. This approach aims to restore the skin's natural ecosystem rather than just suppressing inflammation.
In the future, we may see gene therapies that can "turn off" the signals that cause the skin barrier to be leaky in the first place. Until then, the gold standard remains a combination of diligent moisturization, targeted medications, and lifestyle adjustments. The goal is no longer just to treat the rash, but to achieve clear skin and long-term remission.
Gemini đã nói
Understanding Eczema Treatment: A Comprehensive Guide to Healing Your Skin
Eczema, medically known as atopic dermatitis, is more than just "dry skin." It is a complex, chronic inflammatory condition that affects millions worldwide, characterized by intense itching, redness, and a compromised skin barrier. Finding an effective eczema treatment requires a multi-faceted approach that evolves over time as science advances and as an individual’s skin needs change. This guide explores the journey from immediate relief to long-term management.
1. The Immediate Response: Relieving Acute Symptoms
When an eczema flare-up begins, the primary goal of eczema treatment is to break the itch-scratch cycle. The skin becomes inflamed, leading to microscopic tears that allow irritants and bacteria to enter. Immediate intervention usually involves topical corticosteroids to reduce inflammation quickly and prevent the rash from spreading or becoming infected.
Beyond medication, the first 24 hours of a flare-up require a "back to basics" skincare routine. This involves eliminating all fragranced products and switching to hypoallergenic cleansers. Applying a thick layer of emollient or petroleum jelly immediately after a lukewarm shower helps seal in moisture, providing a physical barrier that the skin currently lacks.
Essential First Steps for Flares
- Identify Triggers: Look for recent changes in soap, detergent, or diet.
- Cool Compresses: Use a clean, damp cloth to soothe burning sensations.
- Antihistamines: While they don't stop the eczema itself, they can help with the sedative effect to ensure better sleep during a flare.
2. Establishing a Daily Maintenance Routine
Consistency is the cornerstone of long-term eczema treatment. Unlike healthy skin, eczema-prone skin loses moisture rapidly through transepidermal water loss (TEWL). A daily maintenance routine isn't just about pampering; it is a medical necessity to repair the stratum corneum, the outermost layer of the skin.
This routine typically centers on the "soak and seal" method. Patients are advised to bathe in lukewarm water for 10 minutes and then apply ceramide-rich moisturizers within three minutes of patting the skin dry. Ceramides are lipids naturally found in the skin that people with eczema often lack, making their replenishment vital for barrier repair.
3. The Role of Topical Prescription Therapies
When over-the-counter lotions aren't enough, doctors prescribe targeted eczema treatment options. Topical calcineurin inhibitors (TCIs), such as tacrolimus or pimecrolimus, are non-steroidal alternatives that work by suppressing the overactive immune response in the skin. These are particularly useful for sensitive areas like the face and eyelids where steroids might cause skin thinning.
Another modern breakthrough in topicals is PDE4 inhibitors. These non-steroidal creams work inside the skin cells to block the enzyme phosphodiesterase 4, which contributes to inflammation. By diversifying the types of topical treatments used, patients can manage chronic symptoms without the long-term side effects associated with continuous steroid use.
Common Topical Categories
- Low-potency steroids: For mild areas or children.
- High-potency steroids: For thick, lichenified (leathery) skin.
- JAK inhibitors (topical): A newer class that targets specific signaling pathways.
4. Understanding Trigger Identification and Avoidance
Long-term eczema treatment is as much about what you don't put on your skin as what you do. Environmental triggers can range from dust mites and pet dander to seasonal pollen. Many patients find that keeping a "skin diary" helps them correlate flare-ups with specific environmental factors or high-stress periods.
Contact irritants are also a major hurdle. Common culprits include sodium lauryl sulfate (found in many soaps) and synthetic fragrances. Switching to 100% cotton clothing and using double-rinse cycles for laundry can significantly reduce the chemical burden on the skin, allowing the natural healing process to take place more effectively.
5. Phototherapy: Harnessing the Power of Light
For patients with moderate-to-severe eczema who do not respond well to creams, phototherapy (light therapy) is a highly effective eczema treatment. This involves exposing the skin to controlled amounts of Narrowband Ultraviolet B (NB-UVB) light. The light waves help reduce the inflammatory response and can even boost the skin's natural antimicrobial peptide production.
Phototherapy usually requires visiting a clinic two to three times a week. Over a period of several months, the skin's appearance improves, and the frequency of flares decreases. It is often used as a "bridge" therapy to get a patient's skin under control before transitioning back to a strictly topical regimen.
6. Advanced Systemic Treatments and Biologics
In the last decade, eczema treatment has been revolutionized by biologic medications. Unlike broad immunosuppressants, biologics like Dupilumab target specific proteins (interleukins IL-4 and IL-13) that are responsible for the underlying inflammation in atopic dermatitis. This "precision medicine" approach allows for clearing the skin with fewer systemic side effects.
For those who prefer oral medications, JAK inhibitors (Janus kinase inhibitors) have emerged as a powerful tool. These pills work by interfering with the signals that tell the immune system to create inflammation and itch. While these systemic therapies require closer monitoring by a dermatologist, they offer life-changing relief for those with refractory eczema.
7. Natural and Integrative Approaches
Many individuals seek a holistic eczema treatment to complement their medical prescriptions. Coconut oil, for instance, has been shown in studies to reduce the presence of Staph bacteria on the skin while providing hydration. Similarly, colloidal oatmeal baths are a time-honored way to soothe irritation and restore the skin's pH balance.
Dietary changes are frequently discussed in the eczema community. While not everyone has a food-triggered flare, some find relief by following an anti-inflammatory diet rich in Omega-3 fatty acids (found in salmon and flaxseeds) and probiotics. These "gut-skin axis" interventions aim to lower the overall systemic inflammation in the body.
8. Managing the Psychological Impact of Eczema
Effective eczema treatment must address the mind as well as the body. The "itch-scratch-anxiety" cycle is real; chronic itching can lead to sleep deprivation, which increases stress, which in turn triggers more eczema. Cognitive Behavioral Therapy (CBT) and habit-reversal training are increasingly used to help patients stop the subconscious urge to scratch.
Support groups and counseling provide an emotional outlet for the frustration that comes with a visible skin condition. Addressing the mental health component of eczema can improve a patient’s adherence to their skincare routine and overall quality of life, making it an essential pillar of a comprehensive treatment plan.
9. Pediatric Eczema: Special Considerations for Children
Treating children requires a gentler touch and a focus on long-term safety. Pediatric eczema treatment emphasizes "wet wrap therapy," where a medicated cream is applied, followed by a layer of damp gauze and a dry outer layer. This increases the absorption of the medication and prevents the child from scratching the area during the night.
Education for parents is vital. Understanding that eczema is not contagious and that it often improves as the child's immune system matures provides much-needed hope. Doctors often focus on maintaining the acid mantle of a child's skin through soap-free cleansing to prevent the development of other allergies, a phenomenon known as the atopic march.
10. The Future of Eczema Care and Prevention
The landscape of eczema treatment is rapidly shifting toward prevention and personalized care. Researchers are currently investigating microbiome transplants, where "good" bacteria are applied to the skin to crowd out harmful pathogens. This approach aims to restore the skin's natural ecosystem rather than just suppressing inflammation.
In the future, we may see gene therapies that can "turn off" the signals that cause the skin barrier to be leaky in the first place. Until then, the gold standard remains a combination of diligent moisturization, targeted medications, and lifestyle adjustments. The goal is no longer just to treat the rash, but to achieve clear skin and long-term remission.
Summary Table: Eczema Treatment Options
Treatment TypeExamplesBest ForTopicalSteroids, Crisaborole, ProtopicMild to moderate local flaresPhototherapyNB-UVB LightChronic, widespread eczemaSystemicMethotrexate, CyclosporineSevere, resistant casesBiologicsDupilumab, TralokinumabTargeted long-term controlOral JAKsUpadacitinib, AbrocitinibRapid itch relief and clearing
Conclusion
Navigating the world of eczema treatment can be overwhelming, but the options available today are more effective than ever before. From the simple act of applying a ceramide cream to the advanced technology of biologic injections, there is a path to relief for every patient. By working closely with a dermatologist and staying consistent with a daily routine, it is possible to move beyond the discomfort of itchy skin and regain confidence in your health.